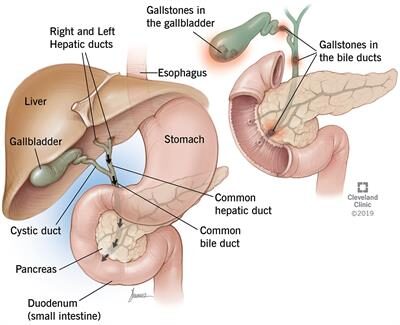
What are Gallstones?
Gallstones are stone-like objects that develop in the gallbladder or bile ducts. Gallstones can be tiny grains of sand ton large lemon shaped. Gall stones can move out of the gall bladder and get stuck in the ducts causing complications or the larger one can stay in the gallbladder and cause inflammation or can get impacted leading to serious complications.
Sometimes gallbladder stones remain asymptomatic for life long.
Types of Gallstones
• Cholesterol: most common type of gallstones.
• Pigment Stones (mainly made of bilirubin): This
substance is created when red blood cells break down in the liver.
Where Do Gallstones Develop?
Gallstones are most commonly found in the gallbladder, as cholesterol stones. Gallstones can also travel from the gallbladder to the common bile duct, which is the largest of the ducts (pipes) in the liver. Common bile duct stones are much less common than gallstones. Stones that find their way into the common bile duct can create more serious medical situations than just gallstones that remain in the gallbladder. Common bile duct stones can block the common bile duct, resulting in a serious infection called cholangitis. These stones can also cause pancreatitis, a painful condition caused by inflammation of the pancreas. Stones in the common bile duct can be removed without surgery by using a scope. Removal of the gallbladder requires surgery, which is typically done laparoscopically (a minimally invasive surgical procedure).
Causes
• High concentration of cholesterol or bilirubin in the bile.
• When the gallbladder is lazy and does not completely empty itself of bile.
• Occurring in people with other conditions, like:
• Cirrhosis of the liver
• Blood disorders.
• During pregnancy.
• Rapid weight loss.
Symptoms
• Most gallstones are asymptomatic and do not require treatment.
• Pain in the upper mid abdomen or upper right abdomen.
• Associated pain in the right shoulder.
• Chest pain.
• Nausea and vomiting.
• Repeated similar episodes.
• Jaundice (a yellow tint to the skin and eyes).
Gallstones can cause acute cholecystitis, which is a more serious condition when the gallbladder is actually inflamed. This happens if a stone blocks off the cystic duct, which increases the pressure within the gallbladder. This condition may require antibiotics, hospitalization, and even urgent surgery. Stones that pass out of the gallbladder and into the
common bile duct can cause a complete blockage of the duct with jaundice, infection, and pancreatitis.
• Upper part of the abdomen, on the right side.
• Between the shoulder blades.
• Under the right shoulder.
Some gallbladders contain a thick sludge, which has not formed into actual stones. Sometimes sludge is felt to cause symptoms similar to actual gallstone pain.
Acalculous cholecystitis when the gallbladder becomes inflamed, but no stones are present. This is generally treated by surgical removal of the gallbladder ( LAPAROSCOPIC CHOLECYSTECTOMY).
Who is at Risk for Gallstones?
You may have an increased risk of developing gallstones if you:
• Are a woman.
• Are over the age of 40.
• Have a family history of gallstones (members of your family have had gallstones).
• Are overweight.
• Have lost a large amount of weight over a short amount of time.
• Have diabetes.
• Have Crohn’s disease.
• Eat a diet that is high in fat and cholesterol.
• Take drugs that lower cholesterol.
• Take various medicines including oral contraceptives.
• Have certain blood disorders.
Does My Diet or Weight Place me at Risk for Gallstones?
People who are overweight or planning to lose weight –either through a planned diet program or surgery —
are actually at an increased risk of developing gallstones.
Diagnosis and Tests
The most commonly used test to detect gallstones is an ultrasound.
Stones in the common bile duct usually require MRI known as MRCP for diagnosis
Magnetic Resonance CholangioPancreatography (MRCP):
MRCP can only diagnose common bile duct stones. It cannot remove them. However, MRCP’s advantage over ERCP is that it is the safer alternative.
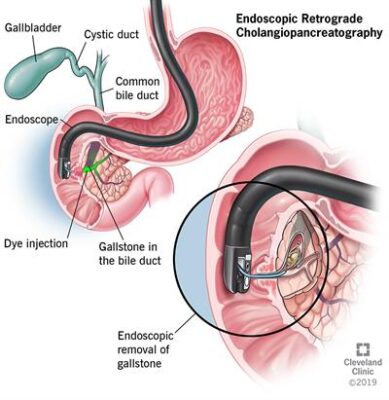
• ERCP: This is both a test and a possible treatment for common bile duct stones. When used as a test, an endoscope—a flexible tube with a light and a camera attached—is inserted into the patient’s mouth, down the throat, and into the stomach and small intestine. A dye is injected to allow the bile ducts to stand out. If there are gallstones in the bile duct, they can be removed by the endoscope.
Endoscopic ultrasound (EUS): This procedure combines endoscopy with ultrasound (there’s a probe at the tip of the scope).
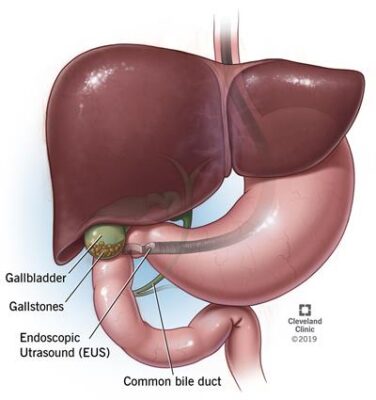
- Illustration showing how the scope of the can go into the body to view the gallstones.
MANAGEMENT AND TREATMENT
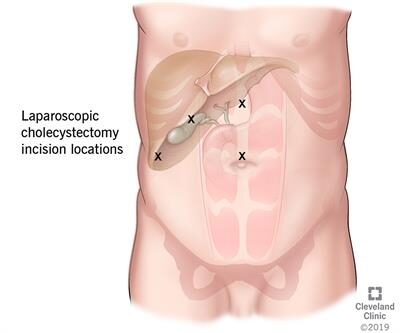
- Illustration of incision locations for a laparoscopic cholecystectomy
Silent stones usually do not require surgical intervention. The most common treatment for gallstones is to remove the gallbladder surgically. Removal of the gallbladder is called a cholecystectomy. In the majority of cases, this surgery can be performed laparoscopically, a minimally invasive technique that results in less post-operative pain and a faster recovery than conventional cholecystectomy. Gallstones that are found in the bile ducts may need
to be removed even if there are no symptoms. This procedure is commonly done with the endoscopic retrograde cholangiopancreatography (ERCP) procedure.
Can I digest food without a gallbladder?
You don’t need a gallbladder in order to digest food properly. If your gallbladder is removed, bile will flow directly from your liver through the hepatic duct and the common bile duct to the small intestine. After the surgery, you may experience some softer stools, which generally resolve over time.
When can I return to my normal activities after laparoscopic gallbladder removal surgery?
If you have a minimally-invasive procedure, you will need a short amount of time to recover before starting your activities again. Patients are usually discharged the next day in the morning and can resume their routine in a day or two.
Two major advantages of minimally-invasive procedures include a much faster recovery time and less pain.
Larger, open surgeries traditionally mean more time in the hospital and a longer recovery at home. Speak with your doctor about a realistic plan for your recovery.
DR ACHAL AGRAWAL
LAPAROSCOPIC, GI & BARIATRIC SURGEON
INDORE LAPAROSCOPY CENTER
- +91-9171770805